Ebola: treating the symptoms but neglecting the cause
Posted on 23 November 2015
West Africa is now largely Ebola-free, but the disease could strike again, according to research by Dr João Nunes in our Department of Politics and International Relations

The issue of Ebola was only noticed when it was presented as a threat to our way of life in the west and the developed north”
The Ebola outbreak made headlines around the world when it raged through West Africa in 2014 and 2015. Vast human, material and financial resources were thrown at a crisis that was termed a “public health emergency” by the World Health Organisation (WHO).
But, according to research by Dr João Nunes in our Department of Politics and International Relations, the Ebola crisis is remarkable not for the amount of attention it received but for the neglect that allowed it to happen – and that could allow it to happen again.
Crisis mode
“The issue of Ebola was only noticed when it was presented as a threat to our way of life in the west and in the developed north,” says Dr Nunes, who is currently writing a book based on his research for publication in 2016. “The world switched into crisis management mode, taking what you might call a vertical approach to the problem, zooming in on the outbreak, seeking to contain and control it but neglecting the broader issues.”
This approach, argues Dr Nunes, ignores the social and economic factors that made this latest in a long series of Ebola outbreaks possible. It is also symptomatic of the inadequate way in which the needs of the local population have historically been addressed – particularly in terms of health provision and infrastructure. If this neglect continues, there is every reason to expect another outbreak of Ebola in the future – a case that Dr Nunes presented recently at a seminar held at the WHO Regional Office for Europe in Copenhagen.
Neglect
“There are no easy fixes to the problem of neglect,” says Dr Nunes. “What we need is a long-term change in global health governance. One place to start would be to give the WHO more control over how to spend its funds. At the moment it is working with its hands tied behind its back because a significant portion of its resources is earmarked by member state donors for particular uses.
“The problem is that the politicians in these donor states are trapped by their own electoral cycles. They are looking for quick results that they can show to their constituents. That ends up meaning that money is spent on short-term projects with easily quantifiable outcomes. But the difficulties we face in global health require long-term strategies.”
Dr Nunes acknowledges that what he is calling for would be controversial. “If the WHO were to pursue its own agenda in addressing the social and economic factors that contribute to health, a lot of people would accuse it of being too politicised – of serving some sort of socialist agenda. “But,” argues Dr Nunes, “the organisation does need to have a political vision, and it needs to be championed by someone with the charisma to bring world leaders together, establish compromises and mobilise public opinion.”
If the WHO could be given more freedom, Dr Nunes believes it is well placed to tackle the causes of neglect. “One of the WHO’s strengths is that it has been designed to work through consultation with its regional offices,” he explains. “It is well placed to harness local knowledge, empowering the actors on the ground rather than imposing an agenda. The more it does that, the less likely it is that local needs will be neglected.”
Primary healthcare
One area that Dr Nunes believes the WHO could do much more on is primary healthcare. Next year he is working on a research programme funded by the Wellcome Trust, looking at the role of community health workers in Brazil. He explains: “Community health workers are not medically trained – they receive basic training in monitoring health and data collection and providing advice – but they are people who have worked with these communities for years.
“They know the families because they visit them regularly, often on a weekly basis, so they have this level of trust. They are able to gather information that would be invisible to traditional doctors. That way the needs of the community can be used to help shape the care provided. I think this kind of primary healthcare provision is one of the ways in which you could really start to tackle neglect.”
There are many who believe that the WHO is part of the problem rather than the solution. The organisation, Dr Nunes is quick to admit, came in for a great deal of criticism for its handling of the Ebola crisis. However he believes it has an essential role to play in the fight against neglect.
Easy target
“The WHO is an easy target. In the Ebola outbreak it was criticised for being too slow to declare a public health emergency. But rewind a few years and it was being accused of the opposite – of jumping the gun on swine flu and creating alarm.
“Of course there have been mistakes, but the WHO is one of the main proponents of the idea of health as a collective issue and a global public good. If it can gain more autonomy – if the democratic voice of its World Health Assembly can have a greater say in what the organisation’s priorities should be, rather than the most powerful member states and donors determining the agenda – then I believe the WHO is our best hope for improving global health."
The text of this article is licensed under a Creative Commons Licence. You're free to republish it, as long as you link back to this page and credit us.

Dr João Nunes
Research interests in international security and the politics of health including neglected issues in global health and health security
Discover the details
- Is Disease a Threat to International Security? was published in The International Relations and Security Network
- WHO must remain a strong global health leader post Ebola (letter) was published in The Lancet
Explore more research
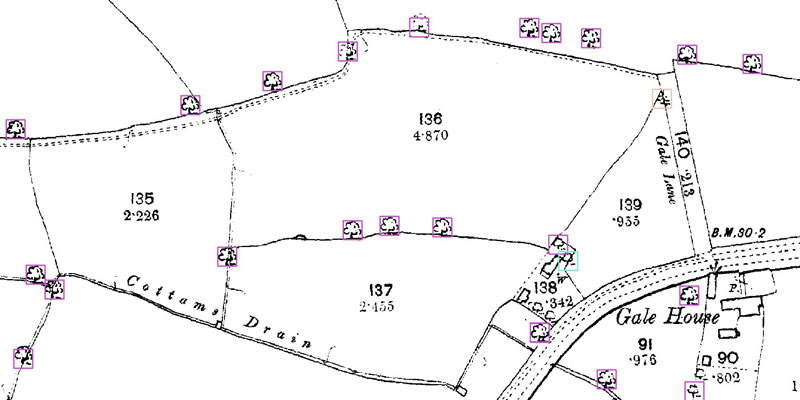
A research project needed to spot trees on historic ordnance survey maps, so colleagues in computer science found a solution.

We’re using gaming technology to ensure prospective teachers are fully prepared for their careers.

A low cost, high-accuracy device, could play a large part in the NHS's 'virtual wards'.
Research newsletter
Our monthly research newsletter features a curated mix of news, events, and recent discoveries delivered straight to your inbox.
