Blood test breakthrough offers hope in the fight against lung cancer
Posted on 20 January 2016
After a decade of research, our biologists are a step closer to a simple test for early stage lung cancer
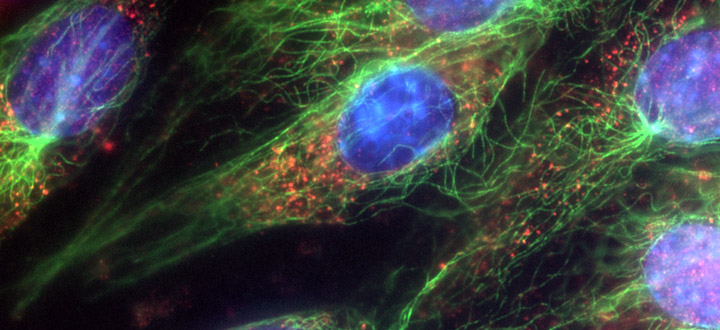
Mammalian cell showing speckles of CIZ1 protein in red in both the nucleus and cytoplasm. Credit: Emma Stewart
The clinical need for this test is huge”
Lung cancer is one of the most common and deadliest forms of cancer, causing over 35,000 deaths in the UK each year. Early detection saves lives but screening options are limited and diagnosis often involves costly biopsies or invasive surgery.
Researchers in our Department of Biology made an important breakthrough in the development of a simple test for the disease when they identified an altered form of a protein called CIZ1 which is present in the bloodstream of lung cancer patients – even when the disease is at a very early stage.
Protein biomarker
Over the last decade, the team proved they could use the protein biomarker to identify patients with very early stage lung cancer under laboratory conditions. But to take the science from the bench to the bedside, they had to find a way to scale up the test to make it compatible for use on a large number of samples in hospital laboratories.
Now, in the last few weeks, they think they may have edged closer to a commercially viable solution.
The work was led by cell biologist Dr Dawn Coverley, who formed a University spin-out company, Cizzle Biotechnology Limited, with the aim of applying her pioneering research in a clinical environment.
“Our biggest challenge has been moving away from the laboratory to a blood test that could be used in high throughput clinical settings,” explains Dr Coverley.
“It’s been tough going. There were no Eureka moments, just a lot of hard work crunching our way through experiments and statistics, but it’s definitely looking more promising.”
Antibodies
The hospital-friendly version of the test is based on an existing scientific technique – known as ELISA – which uses antibodies as tools to detect raised levels of a biomarker. The team at Cizzle have now adapted this technique to detect the variant of CIZ1 that is present in the blood stream of patients with lung cancer.
It’s a significant new milestone which could pave the way for diagnostic trials. But a good deal of scientific hard graft still lies ahead. First the team have to trawl through their banks of sample sets to show that the new blood test method is as reliable as the method developed in the research labs at York.
And then the search begins for a corporate diagnostics company who might be prepared to partner with Cizzle to support large-scale clinical trials and cover manufacturing costs.
“Right now I’m feeling hopeful,” says Dr Coverley. “The clinical need for this test is huge because it’s very difficult for doctors to make decisions about small anomalies that show up on X-rays or CT scans.
Screening programmes
“At the moment, many doctors have to watch and wait in order to avoid unnecessary invasive procedures. What we are working on is a really simple blood test which could be carried out on anybody with suspected lung cancer, possibly in GP surgeries, or it could be developed as part of a screening programme – for instance for all smokers over 60.
“The health benefits of early detection are clear – but there are also economic benefits for the health service.”
Dr Coverley juggles her role as co-founder and chief scientific officer at Cizzle with teaching commitments in the Department. The work at Cizzle, which received support from Yorkshire Cancer Research and commercial investors, takes place alongside fundamental research into the normal function of the CIZ1 protein carried out by post-graduate students Emma Stewart and Rebeca Ridings Figueroa, and post-doctoral scientist Dorian Swartz.
Business case
The team worked with clinicians at New York University Medical School and York District Hospital in a trans-Atlantic alliance that provided the researchers with banks of test material. They hope to work with the University’s Department of Health Economics to build the business case for the blood test.
“We now know that altered forms of the CIZ1 protein are prevalent in the blood of people with tumours in their lungs, and that we can detect it with a relatively simple test. I am hopeful that this will prove valuable in a clinical setting, but it now needs to pass through rigorous clinical trials," says Dr Coverley.
"Whatever the outcome, the science behind our work has the potential to be useful because it gives important new insights into the development of lung cancer – and possibly other forms of cancer.”
Cizzle Biotechnology Limited received support from Yorkshire Cancer Research
The text of this article is licensed under a Creative Commons Licence. You're free to republish it, as long as you link back to this page and credit us.

Dr Dawn Coverley
Research interests in the experimental systems that reconstitute fundamental process associated with DNA metabolism
Discover the details
Yorkshire Cancer Research helps people in Yorkshire avoid, survive and cope with cancer
Publications
- Cyclin A/CDK2 phosphorylation of CIZ1 blocks replisome formation and initiation of mammalian DNA replication was published in the Journal of Cell Science
- Variant Ciz1 is a circulating biomarker for early-stage lung cancer was published in Proceedings of the National Academy of Sciences of the United States of America
Explore more research
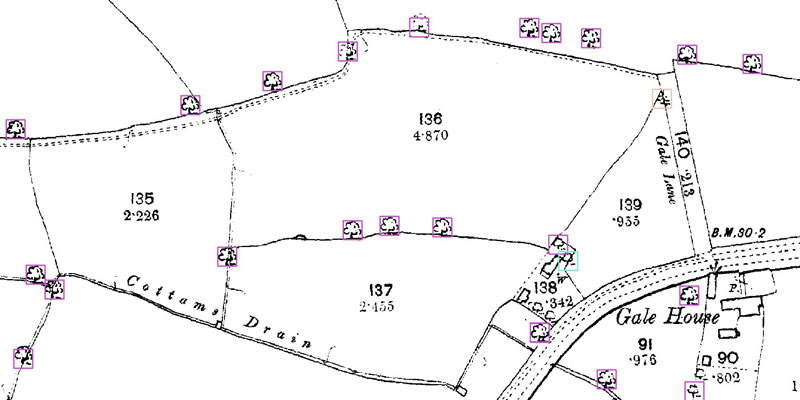
A research project needed to spot trees on historic ordnance survey maps, so colleagues in computer science found a solution.

We’re using gaming technology to ensure prospective teachers are fully prepared for their careers.

A low cost, high-accuracy device, could play a large part in the NHS's 'virtual wards'.
Research newsletter
Our monthly research newsletter features a curated mix of news, events, and recent discoveries delivered straight to your inbox.
