GP health checks offer modest but important benefits for dementia patients
-
Research
- Health and Wellbeing
Posted on 29 March 2016
GPs receive payments for carrying out health checks on dementia patients. But do they represent good value for money? Our health economists examine the evidence...

The effects of the reviews might be modest, but this does not mean they are unimportant”
A national scheme which pays GPs to carry out annual health checks on patients with dementia has brought only a small reduction in emergency hospital admissions for patients suffering from the condition, according to research by our health economists.
But although the benefits of the checks are minimal, the research concludes that they still have an important role for patients and carers dealing with a life-changing condition affecting over 850,000 people in the UK.
“The effects of the reviews might be modest, but this does not mean the review is unimportant – the increasing prevalence of dementia and the constraints on capacity in acute hospital wards may mean even modest impacts are important financially,” says Anne Mason, a senior research fellow in our Centre for Health Economics who led the study.
“While for individual patients the effects may not be substantive, the clinical, social and economic consequences for patients, carers - and society - of fewer and shorter hospital stays are important.”
Quality and Outcomes Framework
Since 2006, GPs have been paid for the annual dementia reviews as part of the NHS Quality and Outcomes Framework (QOF).
The reviews monitor the support needs of patients and their carers. They aim to improve the care of dementia patients, make sure carers are coping with the demands of the illness and help patients stay in their own homes for longer.
The research team at York studied data spanning five years from around 8000 GP practices in England.
As well as identifying a slight reduction in admissions, the research found the GP practices which carry out the highest number of checks achieve slightly shorter than average hospital stays for dementia patients. In addition, these practices record a slightly lower risk of patients being transferred directly from an acute hospital to a care home.
Hospital admissions
“The primary aim of the QOF reviews is not to reduce admissions to hospitals – it is to support patients and carers, but hospital admissions can be considered a measure of the effectiveness of the checks,” says Anne.
“While not all admissions are avoidable, those involving conditions such as angina or respiratory problems could be picked up in GP surgeries as part of the checks and if they are treated well, could reduce the need to go to hospital.
“We found the QOF reviews offered a small protective effect for these types of conditions. It was statistically significant but tiny – so there are some benefits but they are not huge.”
Around one in three people over the age of 65 will develop dementia. Older people with the condition currently occupy nearly a quarter of acute care hospital beds in England.
Further research
Anne would like more dementia patients and carers to know they are entitled to annual checks and she would like to investigate how the reviews are conducted.
“We would like to investigate this in further research. GPs are given guidance on what the reviews should cover, but there have not been any studies looking at what is actually delivered.”
She thinks GPs are uniquely placed to deliver this type of frontline dementia monitoring.
“Even the most articulate, well-educated carer will need help to find out about and co-ordinate different types of care. GPs are uniquely placed to offer this support – they are pivotal to the care of dementia patients in their communities.”
This research was funded by the Department of Health in England, under the Policy Research Unit in the Economics of Social and Health Systems
The text of this article is licensed under a Creative Commons Licence. You're free to republish it, as long as you link back to this page and credit us.

Anne Mason
Research Title: Senior Research Fellow
Research interests in the role of economic incentives in influencing behaviour in the health and social care systems
Discover the details
The Influence of Primary Care Quality on Hospital Admissions for People with Dementia in England: A Regression Analysis was published in PLOS ONE
Bridging the gap: The impact of quality of primary care on duration of hospital stay for people with dementia was published in the Journal of Integrated Care
Visit the Department
Explore more research
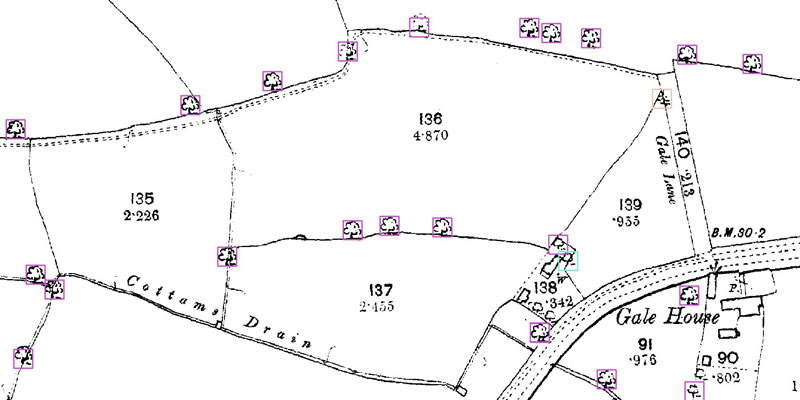
A research project needed to spot trees on historic ordnance survey maps, so colleagues in computer science found a solution.

We’re using gaming technology to ensure prospective teachers are fully prepared for their careers.

A low cost, high-accuracy device, could play a large part in the NHS's 'virtual wards'.
Research newsletter
Our monthly research newsletter features a curated mix of news, events, and recent discoveries delivered straight to your inbox.
