Ethnic Minority/ Global Majority Groups
Projects in this section focus on the inclusion of ethnic minoritised groups in the UK; and global health studies conducted in low- and middle-income countries. We are adding new projects to this section every few months, so please keep checking in to keep up-to-date.
GRT Projects
Project Titles
Crossing boundaries: exploring effective approaches to co-design mental health support with Gypsy, Roma and Traveller communities
Hidden troubles: exploring suicide risk and prevention with Gypsy and Traveller communities
What we’re doing, and why
Hidden Troubles and Crossing Boundaries are a pair of NIHR funded research studies running from 2024-2026, looking at perceptions and experiences of mental health, suicide prevention, and what ‘good’ help looks like for people in Gypsy, Roma and Traveller communities.
People in Gypsy, Roma and Traveller communities are among the most health disadvantaged in the country, even by comparison to other disadvantaged groups. As the communities are often ‘hidden in plain sight’ because of issues of mistrust and discrimination, a lot of what we know is based on partial information and anecdotal information from practice, but evidence suggests that there are high rates of anxiety and depression and a higher likelihood of suicide than in the wider population.
Our projects aimed to build understanding of how communities understood these experiences, what contributed to their experiences, how to build on community strengths and what ‘good’ help might look like.
How we’re doing it:
We’ve reached out to Gypsy, Roma and Traveller communities across Yorkshire and the North East to invite people to take part in one-to-one unstructured interviews, community outreach sessions or activity-focused consultations. Within these sessions, conversation is introduced around three key areas: nature and causes of mental distress, what made help ‘good’, and proposed solutions. Participants lead the discussions, supported by researchers, to focus on community priorities. Data are collected through fieldnotes for analysis using reflexive thematic analysis, which will be workshopped with community members to check relevance.
Research Inclusion: Coproduction with people from Gypsy, Roma and Traveller communities
People from Gypsy, Roma and Traveller communities can be mistrustful of ‘the state’ (including research), linked to previous experiences of mistreatment and discrimination, concern about what will be done with the information they provide, and scepticism that nothing will change. To counter this, our projects were codesigned from the outset, working with two organisations that support a combination of Gypsy, Roma and Traveller communities.
Our research team includes two community members who have taken lead roles in guiding the research, and our ‘on the ground’ research team has included people from English Romany, European Roma, and Irish Traveller communities as well as academic researchers. The wider community were involved in planning discussions through these connections, as we established a group of peer researchers who have supported us in research design, recruitment, data collection, analysis and impact planning.
Team
Our research team is led by Laura Tucker (University of York) and Violet Cannon (York Travellers Trust) and includes community practitioners from York Travellers Trust and Waythrough, academics from York, Northumbria and Bristol, NHS representatives from Tees, Esk and Wear Valley NHS Trust and community members from across Yorkshire and the Northeast.
Find out more on the study websites:
Hidden troubles: exploring suicide risk and prevention with Gypsy and Traveller communities
Image from one of our activity focused consultation events (October 2025)

The SERPENT project
Project title
SERPENT: Skills and Essentials Required to ParticipatE iN the digiTal world#
What we’re doing
This project aims to understand what matters to people with serious mental illness (SMI) who are from culturally diverse or ethnic minority backgrounds when learning digital skills.
We intend to find out what’s important when learning digital skills, and the opportunities and challenges of using online digital courses.
Using co-production we will explore how training and resources can be tailored to be culturally relevant, supportive and useful.
How we’re doing it
Timeframe: 1 September 2025 to 31 March 2026 (7 months)
Series of workshops: People with lived experience of severe mental illness from culturally diverse backgrounds in partnership with Sheffield Flourish (https://sheffieldflourish.co.uk/)
Outputs and Future Plans: Co-designed guidelines and recommendations to inform the development of a future online digital skills course. Develop a future grant application
Research inclusion: Embedding ethnic minority inclusion in a co-production RCF project
People with SMI are more likely than the general population to be subjected to the ‘digital divide,’ defined as lack of access to digital technology or the skills or motivation to use it (Spanakis et al. 2021). Despite evidence from our previous work (Dragon, 2023) which showed that providing tailored support to people with SMI, to use freely available online digital skills courses (https://www.goodthingsfoundation.org/learn/learn-my-way), enabled them to develop foundational skills, the courses were not culturally diverse. The SERPENT project addresses this gap through co-production with people from a range of ethnic minority groups. By collaborating with community organisations such as Sheffield Flourish, the team aims to build long-term trust and ensure meaningful involvement of underserved ethnic minority communities, who are disproportionately affected by digital exclusion.
Project Objectives
* Understand User Needs: Explore the specific preferences, priorities, and digital capabilities of adults with SMI from diverse cultural backgrounds.
* Identify Barriers & Facilitators: Determine what hinders or enables the delivery of digital skills interventions in these communities.
* Assess Impacts on Health: Consider how co-produced tools impact digital health literacy, use of the NHS App, and health-seeking behaviour.
* Inform Future Research: Use these insights to develop and trial culturally appropriate digital inclusion tools through future funding applications.
By embedding inclusion directly into the research framework, SERPENT aims to move beyond ‘one-size-fits-all’ digital resources, creating guidance that is bespoke and culturally resonant.
Team
The core SERPENT team comprises researchers from the Mental Health and Addiction Research Group in the Department of Health Sciences, University of York. Joint PIs, Dr Kate Bosanquet and Dr Trish Darcy, are collaborating with community partners Dr Josie Soutar (Managing Director) and Lisa Thompson-Cox (Community Engagement & Volunteer Coordinator) at Sheffield Flourish. Other contributors include Dr Raihan Talukdar (Consultant Psychiatrist & Chief Clinical Information Officer) and Fiona Czarnecki (Senior Business Architect) at Sheffield Health Partnership University NHS Foundation Trust.
Funder information: This study is funded by Sheffield Health Partnership University NHS Foundation Trust (RCF) and the NIHR Applied Research Collaboration Yorkshire Humber.
The TRUST Study
Project title
Enhancing Gypsy, Roma and Traveller peoples’ trust: using maternity and early years’ health services and dental health services as exemplars of mainstream service provision
What we aimed to do
People who identify as Gypsy, Roma and Travellers (GRT) are a marginalised and socially excluded group. Despite the fact that GRT people constitute a significant minority group in the UK, at the time the TRUST project was undertaken, the evidence base for improving health and access to services within the GRT population was weak.
We aimed to investigate which approaches to community engagement are likely to enhance trust between GRT people and mainstream health services.
How we did it
We conducted a multi-component study that aimed to strengthen the evidence regarding how to improve uptake and delivery of health services and thereby reduce health inequalities for GRT people. The study comprised:
Stage 1: literature reviews to understand GRT engagement with health services, the concept of trust in healthcare settings, and engagement strategies for GRT people in health services.
Stage 2: semi-structured, online consultation to gather views on trust and engagement in health services for GRT people.
Stage 3: case studies to generate in-depth, multi-faceted understanding of the complex issues surrounding enhancing trust and engagement between mainstream health services and GRT communities in their real-life context.
Stage 4: two in person cross-sectoral workshops and a teleconference to sense check study findings and to develop recommendations for policy. Economic evaluation of providing health care interventions to improve accessibility of NHS services by and for GRT communities.
Research inclusion: Gypsy, Roma and Traveller communities
In this project we worked closely with GRT people, organisations and health care professionals that support GRT.
Public and Patient Involvement (PPI) was central to the conception, design, conduct and interpretation. Four strategies were employed:
- The team included the CEO of Leeds Gypsy and Traveller Exchange, a community members’ organisation that works to improve the lives of Gypsies and Travellers in West Yorkshire and beyond.
- A User Advisory Group comprising women representing the Romany Gypsy, Irish Traveller and Eastern European Roma communities met four times during the study and advised on the conduct of the study as well as interpretation and dissemination.
- We held two advocacy training workshops to support the User Advisory Group and the wider GRT community to participate in research.
- We included individuals from third sector organisations who represented and advocated for GRT communities in the online consultation, the case studies, and the Stakeholder workshops.
Team
The TRUST team comprised researchers from the University of Dundee: Professor Alison McFadden, Dr Lindsay Siebelt, Professor Nicola Innes, Dr Stephen MacGillivray, Dr Anna Gavine, Dr Haggi Michael Haggi; University of York: Dr Kerry Bell, Dr Cath Jackson, Professor Karl Atkin, Belen Corbacho; and Helen Jones from Leeds Gypsy and Traveller Exchange.
Professor Alison McFadden was the lead investigator.
The full report from this work is available here: https://discovery.dundee.ac.uk/ws/portalfiles/portal/29156227/McFadden_et_al_GRT_Trust_and_Engagement_Final_report_140918.pdf
This research was funded by the Department of Health Policy Research Programme: PR-R8-0314-24002
DIAMONDS
Project title
Improving diabetes self-management and outcomes for people with severe mental illness
What we did
The NIHR-funded DIAMONDS programme ran from May 2018 – November 2025. The overall aim of the programme was to develop and test a bespoke support and educational package to help people with severe mental illness (SMI) better manage their Type 2 diabetes (T2D) and other long-term physical health conditions.
T2D is more than twice as common among people with SMI compared with the general population. People who have SMI and T2D also tend to be more unwell than people who have T2D without an SMI, and they experience more side effects or complications.
The focus of the project was on Type 2 Diabetes, but the final workstream focused on adapting the intervention for a wider range of physical health problems.
Project Overview
Research inclusion: People living with Severe Mental Illness (SMI) and long-term conditions
The expertise of people with SMI and their carers was integrated into the research of the DIAMONDS Programme, moving beyond passive participation into active co-design.
In Workstream 1, they contributed via interviews to identify the specific barriers to self-managing physical health. In the co-production phase (WS2), they worked alongside researchers to design the intervention’s workbook and app to ensure they were practical and user-friendly. During the feasibility and trial stages (WS3 and WS4), participants provided critical feedback through interviews, allowing the team to refine the intervention based on real-world experience. Workshops with people with SMI and their carers were also integral to Workstream 6, adapting the intervention for further conditions.
DIAMONDS Voice
DIAMONDS Voice is the DIAMONDS Patient and Public Engagement panel. This group of service users and family carers with experience of living with mental and physical health comorbidity met 3-4 times a year to provide input to the DIAMONDS programme.
The group kept the research focussed on important questions for people living with SMI and long-term conditions, and advised on ways to minimise participant burden, the content and format of study documentation, the interpretation of findings, and dissemination for patient and public audiences. Some members have been involved in speaking at conferences, disseminating information through public sector networks, and co-authoring publications.
The group was facilitated by co-ordinator Angie Ross, and was a vibrant and vital part of the DIAMONDS project.
Team
The DIAMONDS programme was a joint venture between the University of York and Bradford District Care NHS Foundation Trust. The team was led by PI Professor Najma Siddiqi (York), drawing on expertise from the universities of Leeds, Dundee, UCL and Southampton, with collaborators also from Kings College London, HYMS, Leicester Diabetes Centre, and Valid Research. The programme was managed by Dr Jennifer Brown.
You can see more details here: https://www.york.ac.uk/healthsciences/research/mental-health/projects/diamonds/diamonds-involved/

The DIAMONDS Voice group (as seen on DIAMONDS Voice)
Find out more on the study website: https://www.diamondscollaboration.org.uk/
Funder information: This study was funded by the National Institute for Health and Care Research (NIHR), Programme Grants for Applied Research Programme (RP-PG-1016-20003).
Older South Asian people
Project title
Perceptions and experiences of older South Asian people about participating in health and care research
PhD candidate: Lubena Mirza
Lubena started working on her PhD (part-time) in 2023, alongside her role as a Research Fellow at the Bradford Institute for Health Research. Her projects focus on the wellbeing and safety of older people in community and hospital settings. She is a proponent of qualitative methodologies and is also experienced in participatory research, including co-design. Her research interests include research inclusivity for people of minoritised backgrounds and the agency of older people around research involvement.

Research inclusion: older South Asian people
South Asian people are underrepresented in health and care research but disproportionately affected by comorbidities. There is a wealth of literature exploring barriers and facilitators to conducting inclusive research, highlighting how views and experiences of research shape willingness to be involved, including fears, motivations, sense of belonging and trust. However, we know little about how older (65+) people of South Asian backgrounds – particularly Indian, Bangladeshi and Pakistani backgrounds – view and experience research. Exploring how research is perceived and experienced by this population will help us understand how to make research more inclusive.
How this research is being done
Study 1: A scoping review of the literature, to explore what we already know about the views and experiences of older South Asian people and their participation in research. This research will map these views and experiences, in terms of how that research was carried out (e.g. interviews and focus groups), who is represented in that research (e.g. age, gender and other demographic details); and where that research was done including setting and country.
Study 2: Focus groups with older South Asian people and carers living in the Leeds and Bradford areas. The researcher conducted focus groups in Urdu, Punjabi and Bengali, and ran separate focus groups for men and women.
Study 3: A qualitative study involving interviews with key informants (for example community or religious leaders). These conversations will enable insights into their experiences, and the stories and messages they hear from older South Asian people around participating in research.
Team
Researcher: Lubena Mirza, Department of Health Sciences, University of York
Supervisors: Professor Joy Adamson and Dr Suman Prinjha, Department of Health Sciences, University of York
The UPTURN study
What we’re doing
UPTURN is a 5-year NIHR-funded study that aims to support people with Chronic Obstructive Pulmonary Disease. COPD is a common lung condition in which airflow is obstructed. It causes breathlessness, persistent cough, wheezing and other symptoms.
Pulmonary Rehabilitation, or PR, is the most effective treatment for COPD symptoms and includes tailored, supervised exercise and education. Research shows that PR is very effective in helping people better manage the condition at home, but uptake of PR sessions is low. There can be many reasons for this.
Up to one third of COPD patients don’t attend their initial PR assessment or take up the programme, and so never get the benefit of the treatment. 90% of people who do attend the PR assessment go on to attend PR sessions.
UPTURN aims to help more people attend their PR assessment. We’re doing this by co-designing a new PR support package, working with people living with COPD, their families, and healthcare professionals.
How we’re doing it
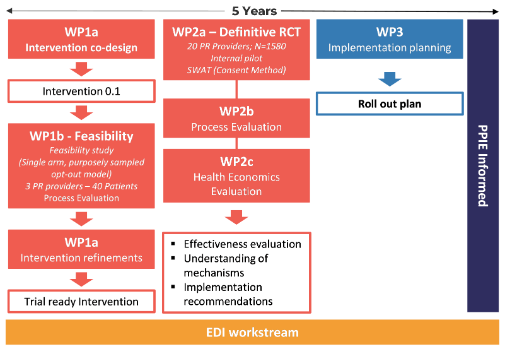
Research inclusion: Embedding ethnic minority inclusion in a clinical trial
COPD disproportionately affects some ethnic minority groups. UPTURN has an EDI Workstream that runs throughout the study. The Workstream supports every aspect of the project including community engagement, intervention codesign, recruitment to qualitative and clinical trial research, training, capacity building, and dissemination.
The EDI Workstream team focuses on the meaningful involvement of Bangladeshi, African and Caribbean communities, who are unequally impacted by COPD. The EDI team is led by five researchers from diverse backgrounds, with a range of cultural and linguistic knowledge to contribute to every phase of the work.
The EDI team is building long-term relationships with community organisations to raise awareness of COPD and improve health literacy. Five PPI Groups help support the work: a broad group for everyone, and smaller community-specific groups for Bangladeshi men, Bangladeshi women, African communities, and Caribbean communities. The team regularly blogs about its Research Inclusion journey.
Team
The EDI Workstream Team is based at York Trials Unit and helps to ensure that Research Inclusion is embedded throughout the project. It’s led by Dr Suman Prinjha, who works with four Community Researchers: Dr Ada Achinanya, Lorraine Lawrence, Dr Rabbani Golam, and Dr Tahsin Tabassum.

Left to right: Lorraine Lawrence, Tahsin Tabassum, Ada Achinanya, Suman Prinjha, Rabbani Golam
The UPTURN team comprises researchers from various UK universities. The full team of applicants:
Dr Jonathan Fuld, Chief Investigator, Cambridge University Hospitals NHS Foundation Trust; Professor Stephen Morris, Co-Chief Investigator, University of Cambridge; Dr Suman Prinjha, University of York; Mr Jeff Andrews, PPI lead; Mr Mir Gofur, PPI lead; Miss Tracy Cripps, PPI lead, Cambridge University Hospitals NHS Foundation Trust; Professor Fabiana Lorencatto, University College London; Dr GM Monsur Habib, Bangladesh Primary Care Respiratory Society; Dr Jamie Murdoch, King's College London; Professor Lee Shepstone, University of East Anglia; Mr Mike McKevitt, Asthma + Lung UK; Professor P John Clarkson, University of Cambridge; Dr Polly-Anna Ashford, University of East Anglia; Professor Sally Singh, University of Leicester; Dr Stephen Holmes, NHS Somerset Integrated Care Board
Find out more on the study website: https://www.upturn-study.co.uk
Funder information
This study is funded by the National Institute for Health and Care Research (NIHR), Programme Grants for Applied Research Programme (NIHR204401).
The SAME Study
Project title
Exploring the barriers and facilitators to sustained engagement with mental health services for South Asian people.
What we’re doing
The South Asian Mental health service Engagement (SAME) Study is a qualitative study which has been funded by the Tees, Esk and Wear Valleys (TEWV) NHS Foundation Trust and is being run by a research team based at the University of York.
The primary objective of the study is to understand more about how South Asian people engage with local mental health services. We know that South Asian people are less likely to seek help for their mental health problems for many reasons including cultural stigma and shame, as well as language barriers and lack of adapted services. Additionally, those that access these services are less likely to stay engaged for a long enough period of time to improve their mental health.
We hope that by learning more about these experiences, we will understand what services are already doing well and what can be improved for South Asian people. This knowledge may help to develop new ways in which we can adapt existing services which are delivered to South Asians so they are easier to use and more likely to improve their mental health.
How we’re doing it
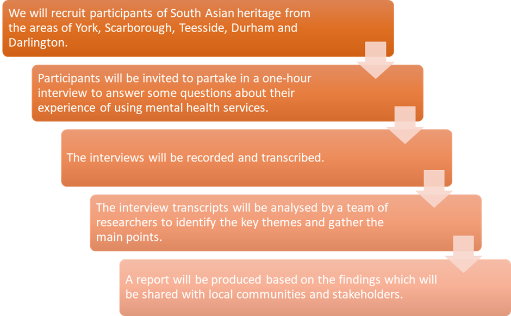
Research inclusion: Embedding ethnic minority inclusion in a qualitative study
We know from previous research that South Asian people in the UK experience a variety of different socioeconomic challenges such as poorer educational opportunities, poverty and unemployment which may be contributing to the higher rates of mental health problems seen in this population. With South Asians less likely to use mental health services, this creates a growing problem for this group.
Although it is the largest ethnic minority in the UK, there are fewer South Asian people living in North Yorkshire and the North East, therefore they may experience more unique challenges with regards to engaging with local mental health services compared to more diverse areas of the UK which may already have cultural adaptations in place.
However, the same barriers that reduce access to mental health care for South Asian communities also exist within research. South Asian people are less likely to take part in research than the wider population, and so we are collaborating with local community groups such as the York Indian Cultural Association to foster real connections and build a level of trust that we hope will lead to further involvement of local South Asian communities.
We have also developed a PPI group made up of South Asian people from different backgrounds with a range of professional and personal experience. They are playing a pivotal role in ensuring the project is culturally appropriate.

Team
The research is being carried out in the Department of Health Sciences, University of York, and is led by Dr Kavindu Appuhamy, an Academic Clinical Fellow in Psychiatry. He is joined by Dr Hannah Jennings, Dr Gerardo Zavala, and Dr Rabbani Golam from the University of York; Ayesha Khaliq from the University of Manchester, and Dr Hassan Awan from Keele University.
Funder information
This study is funded by the TEWV NHS Foundation Trust through the National Institute for Health and Care Research (NIHR) Research Capability Funding.
Global Health Projects
DiaDeM
Project title
Developing and evaluating an adapted behavioural activation intervention for people with depression and diabetes in South Asia
What we did
Type 2 diabetes is a growing global problem, particularly in South Asia. People with long-term physical health conditions, such as diabetes, are more likely to experience depression. When people have depression and diabetes, outcomes for both are worse, resulting in poorer health and quality of life, earlier deaths, and increased costs for individuals, families and healthcare services.
DiaDeM was a 4-year NIHR-funded programme that brought together experts in the field to develop and test a culturally appropriate treatment for depression in people with diabetes in Bangladesh and Pakistan.
The programme received follow-on funding from the NIHR in 2025 to implement the Behavioural Activation (BA) intervention and its training package, both locally at the sites at which the trial was run, and in other healthcare settings in Bangladesh and Pakistan where there is a high prevalence of unaddressed depression.
How we did it
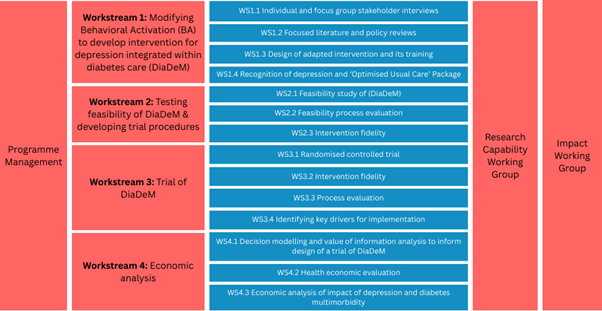

The Workstreams of the DiaDeM programme
Research inclusion: Low- and Middle- Income Countries and mental illness
The DiaDeM programme prioritised the meaningful inclusion of vulnerable populations through a robust Community and Public Involvement (CPI) framework guided by the principle "Nothing About Us Without Us". To ensure the research was grounded in local realities, Local Community Panels (CPs) were established in Bangladesh and Pakistan, consisting of people living with depression and diabetes, their caregivers, and community influencers such as religious leaders and teachers.
These panels were involved at every stage of the project, from the initial proposal and co-design of the intervention to evaluation and dissemination. The programme actively sought feedback via workshops and focus groups to identify and mitigate barriers to participation, such as health system constraints and cultural sensitivities. By integrating these "lived experience" perspectives, DiaDeM ensured that research priorities and the intervention materials were culturally appropriate, feasible, and directly beneficial to those living with complex multi-morbidity in LMIC settings.
Team
Led by PI Professor Najma Siddiqi (York), the DiaDeM Programme and its follow-on work brought together UK partners from Universities of Leeds and Southampton, University College London, and Tees, Esk & Wear Valley NHS Foundation Trust, as well as international collaboration from:
- Bangladesh: The ARK Foundation and the Diabetic Association of Bangladesh (BADAS).
- Pakistan: Khyber Medical University, the Institute of Psychiatry, PPHI Sindh and Indus Hospital & Health Network.
- Europe: The Luxembourg Institute of Socio-Economic Research.
Together, these partners form a global network dedicated to addressing the intersection of diabetes and depression through diverse clinical and socioeconomic perspectives.

DiaDeM Dissemination Event, July 2025 (see more here)
Find out more on the study website: https://www.impactsouthasia.com/diadem/
Funder information
This study was funded by the National Institute for Health and Care Research (NIHR), Research and Innovation for Global Health Transformation (RIGHT) Programme (NIHR200806).
COPE-BP
Project Title
Community-Pharmacies managing hypertension: intervention development and evaluation in Bangladesh and Pakistan (COPE-BP).
What we are doing
COPE-BP is a 5-year global health research programme (2025–2030) addressing the critical burden of uncontrolled hypertension in Bangladesh and Pakistan. In these countries, over 60% of people with hypertension remain undiagnosed or untreated, contributing to high rates of cardiovascular disease.
The project specifically targets Low-Income Urban Residents (LIURs) who often lack access to formal primary care. We aim to develop and test a scalable, community-based intervention where pharmacists—often the first point of contact for health advice—collaborate with physicians to manage blood pressure effectively.
How we are doing it
The research is structured into six integrated work packages (WPs) to ensure the intervention is effective, sustainable, and scalable:
- WP1: Intervention Development:
A mixed-methods approach (geo-mapping, surveys, interviews) to co-design the intervention with patients, pharmacists, physicians, caregivers, and policymakers.
- WP2: Feasibility Assessment:
A cluster Randomised Controlled Trial (cRCT) to test recruitment and data collection processes.
- WP3: Evaluation (Main Trial):
A large-scale pragmatic cRCT comparing the COPE-BP intervention against usual care to assess blood pressure control over 24 months.
- WP4: Process Evaluation:
Assessing implementation mechanisms (barriers and facilitators) to understand how the intervention works in different local contexts.
- WP5: Economic Evaluation:
Analysing cost-effectiveness to demonstrate value for money and support future scalability.
- WP6: Capacity Building:
Upskilling community pharmacists and developing academic leadership in Bangladesh and Pakistan.
Research Inclusion: low-income urban residents in Bangladesh and Pakistan
COPE-BP is committed to "Research for the Community, by the Community." Our inclusion strategy addresses the severe health disparities faced by urban poor populations.
We specifically work with low-income urban residents in both the countries. These groups are often excluded from formal healthcare due to cost and location.
We have established Community Advisory Panels (CAPs) in both Bangladesh and Pakistan, comprising patients, caregivers, and community leaders. They actively advise on study design, ensuring materials are culturally appropriate and accessible (e.g., translated into Urdu and Bangla).
We actively promote gender equity by training female community pharmacists and ensuring our data collection captures the specific barriers faced by women in accessing cardiovascular care.

Glimpses from the Community Advisory Panel (CAP) meetings in Bangladesh and Pakistan
Project Impact
- Health Impact: Potentially improving control for 35 million people and preventing approx. 62,000 deaths annually in Bangladesh and Pakistan.
- System Impact: Creating a blueprint for integrating community pharmacies into national health systems to manage non-communicable diseases.
Team
The project is led by Dr Saima Afaq and is a collaborative effort between six key partner organisations:
- University of York (UK)
- ARK Foundation (Bangladesh)
- Khyber Medical University (Pakistan)
- University of Oxford (UK)
- University of Glasgow (UK)
- Valid Research Pvt. Ltd. (UK)

The COPE-BP team in its First Annual Meeting in Istanbul (10th December, 2025)
Funder Information
This study is funded by the National Institute for Health and Care Research (NIHR) [Ref: NIHR206976].
Global Equity in Research
Project Title
Global Equity in Research: Fostering Women’s Leadership and Decolonisation in the Global South.
What we did
Global health research is often characterised by significant power imbalances, largely driven by the Global North. This disparity disproportionately affects women scholars in the Global South, who face a double burden of gender inequity and colonial research structures.
Building on the work of the Centre for IMPACT, this project aimed to critically re-evaluate these structures. Our specific goal was to understand the lived experiences of women researchers in Afghanistan and Pakistan—two challenging contexts for female leadership—and to co-develop a strategy to dismantle barriers to their progression.
How we did it
We utilised a participatory, co-design approach to ensure the solutions were rooted in real-world experiences.
- Participatory Workshops: We conducted a series of four in-depth workshops with women scholars at various career stages in Afghanistan and Pakistan.
- Vignettes (Storytelling): From these discussions, we developed "vignettes"—anonymised narratives that captured specific challenges regarding leadership, authorship, and funding.
- Co-creation: Using these vignettes as a catalyst, the team worked with stakeholders to identify practical solutions.
- Toolkit Development: We have translated these findings into a practical "Global Equity in Research Toolkit." This resource provides actionable guidelines for institutions to promote inclusive research cultures.

Gender Equity in Research Workshop at the Khyber Medical University, Pakistan
Research Inclusion: women researchers in Afghanistan and Pakistan
This project is explicitly centered on Equality, Diversity, and Inclusion (EDI) and the Decolonisation of Global Health.
- We focused on the intersection of gender and geography, addressing how "Global South" status compounds gender discrimination.
- The methodology was designed to amplify voices that are usually silenced in academic discourse.
Project Impact
- The toolkit serves as a global resource to aid research culture transformation, emphasising gender equity.
- The project aims to increase the number of grants and manuscripts led by women scholars in the region.
- The core strategy group has been integrated into the Centre for IMPACT’s governance structure (running until 2027) to ensure long-term commitment to these principles.
Team
The project is led by Dr Saima Afaq and is hosted by the Centre for IMPACT (University of York), involving collaboration between:
- University of York (UK)
- Mahidol University (Thailand)
- Khyber Medical University (Pakistan)

Project team presenting at the Centre for IMPACT’s Annual Meeting in Abbottabad, Pakistan
Funder Information
This work is supported by the Wellcome Trust under the "Valuing Voices for Equitable and Responsible Research" funding call.
The POTENTIAL
Project Title
Improving outcomes in people with TB by integrating diabetes prevention and management in TB care (The POTENTIAL)
What we did
The POTENTIAL project (2022–2025) addressed the critical double burden of Tuberculosis (TB) and Diabetes Mellitus (DM) in Pakistan. Pakistan ranks globally among the highest for both diseases, and their co-occurrence creates a severe public health threat, leading to treatment failure, relapse, and increased mortality.
Our primary goal was to dismantle the silo approach of traditional healthcare. We developed and tested a TB-Diabetes Care Package, an integrated model where diabetes management is embedded directly into existing TB control programmes. This ensured that patients receiving TB treatment were simultaneously screened and treated for diabetes, providing holistic, patient-centred care.
How we did it
We utilised a sequential mixed-methods design to ensure the intervention was evidence-based and scalable:
- Contextual Analysis: We conducted a needs assessment, including a rapid appraisal to map the gaps in the existing TB-DM care landscape.
- Intervention Co-design: Using Implementation Mapping (IM) approach, we co-produced the care package with stakeholders. This included developing clinical manuals, patient education tools, and training modules for frontline workers.
- Feasibility Testing: We conducted a feasibility study in four TB centers. This evaluated the practical challenges of delivery.
- Definitive Implementation Study: We conducted a full implementation study across five districts in two provinces (Khyber Pakhtunkhwa and Punjab in Pakistan), and assessed the reach, effectiveness, adoption, implementation, and maintenance of the care package.
Research Inclusion: TB patients in Pakistan
Our inclusion strategy focused on the specific vulnerabilities of TB patients in Pakistan, who often face poverty and social stigma.
- We targeted patients in public sector TB clinics, who are often from lower socio-economic backgrounds and cannot afford private diabetes care.
- The intervention was designed with direct input from patients to ensure the added diabetes care did not become a burden. We prioritised one-stop services to reduce travel costs and time for patients.
- By involving the National TB Control Programme from day one, we ensured that the research was not just academic but designed for real-world policy adoption.

TB-diabetes guidelines development workshop at the Rawalpindi Medical University Pakistan
Project Impact
- Delivered a validated manual and training guide for integrating diabetes care into TB services.
- Generated key evidence and recommendations to support the National TB Control Programme in updating guidelines to manage comorbidities.
- Upskilled healthcare workers in the management of complex dual-disease presentations.
Team
The project was a collaborative effort led by Dr. Saima Afaq, and is hosted by Khyber Medical University (Pakistan) in partnership with:
- University of York (UK)
- Rawalpindi Medical University (Pakistan)
- Baqai Institute of Diabetology and Endocrinology (Pakistan)
- Aga Khan University (Pakistan)
- National TB Control Programme (Pakistan)
The POTENTIAL field team with the Principal Investigator Dr. Saima Afaq
Funder Information
This study was funded by the Higher Education Commission (HEC) of Pakistan under the Grand Challenge Fund [Ref: 20-GCF-770].
SCIMITAR-SA
Project title
The SCIMITAR-South Asia programme to address tobacco-related multiple long-term conditions in Severe Mental Illness
What we’re doing
The NIHR-funded SCIMITAR-SA project investigates methods of treating tobacco dependence among individuals in South Asia with the most severe forms of mental illness. It will run for four years: 2024-2028.
How we’re doing it

Research inclusion: People living with Severe Mental Illness in LMICs
The SCIMITAR-SA programme ensures the meaningful inclusion of people living with severe mental illness (SMI) across India, Bangladesh, and Pakistan through a structured Community Engagement and Involvement (CEI) framework that prioritises collaboration and community ownership.
Central to this approach is the CEI Working Group which, while identifying and addressing barriers for underrepresented groups, integrates diverse community voices into every stage of the research: from planning and implementation to evaluation. The project has Community Advisory Panels (CAP), whose members act as a bridge between research teams and the local population, providing essential feedback on project design and participating in collaborative training developed across all three countries.
SCIMITAR-SA empowers participants and their families by treating caregivers as "change makers" and providing them with structured psychoeducation and communication tools to support tobacco cessation and recovery. This inclusive model is underpinned by ethical principles that safeguard participant autonomy and dignity, ensuring that research remains transparent, respectful, and focused on the practical needs of the community.
Team
The SCIMITAR-SA project is co-led by Professor Simon Gilbody (York) and Professor Pratima Murthy, Professor of Psychiatry, National Institute of Mental Health and Neurosciences (NIMHANS) Bangalore, India. It is a collaboration between the University of York, NIMHANS, and organisations in Pakistan, India, and Bangladesh, including:
- ARK Foundation (ARK) Bangladesh
- DMKM Community Healthcare Initiatives and Priorities (CHIP) LLP
- Institute of Psychiatry (IoP) Pakistan
- Pakistan Institute of Living & Learning (PILL)
You can see more details here: https://www.impactsouthasia.com/scimitar-sa/about-us/meet-the-people/

Find out more on the study website: https://www.impactsouthasia.com/scimitar-sa/
Funder information
This study is funded by the National Institute for Health and Care Research (NIHR) Research & Innovation for Global Health Transformation (RIGHT) programme (NIHR205601).
TB-Anxiety
Project Title
Integrating Anxiety Care in Tuberculosis Services in Pakistan
What we did
This study addressed the urgent but often-overlooked mental health crisis within tuberculosis (TB) care. While the physical symptoms of TB are treated, the psychological toll is severe—up to 80% of active TB patients experience anxiety, which threatens treatment adherence and recovery. Currently, Pakistan's National TB Control Programme only provides mental health support for Multi-Drug Resistant (MDR) TB, leaving the vast majority of patients—those with Drug-Sensitive TB (DSTB)—unsupported.
Our goal was to bridge this gap by exploring how anxiety is currently managed in routine TB clinics and assessing the acceptability of an Integrated Anxiety Care Package for all TB patients.
How we did it
We conducted a rigorous qualitative study involving face-to-face semi-structured interviews with key stakeholders across the healthcare spectrum in Pakistan.
- Participants: We interviewed 19 healthcare workers, 1 service manager, 12 patients with DSTB, and 9 caregivers.
- Analysis: Using the "Framework Method," we analysed the data to understand the lived experiences of patients and the operational realities of health workers.
Key Findings:
- The Treatment Gap in Routine Care:
Our primary findings revealed that while anxiety is recognised as a major issue, it is currently not managed effectively:
- There are no formal guidelines or screening tools for anxiety in DSTB patients. Healthcare workers currently offer only informal advice or general counselling, which they feel is insufficient.
- Health workers identified a lack of time, training, and referral pathways as major barriers preventing them from supporting patients' mental health.
- There was a high level of acceptability for the proposed care package. Both patients and health workers strongly agreed that anxiety screening and counselling should be a standard part of routine TB visits, rather than a separate service.
- The Gender Dimension:
Our analysis further revealed stark gender disparities in how TB and anxiety are experienced:
- Women reported significantly higher levels of anxiety and depression, often linked to a double stigma of having an infectious disease while being female.
- Unmarried women feared a TB diagnosis would destroy their marriage prospects, leading to concealment of the disease. Married women often feared rejection or separation from their children.
- Female caregivers (daughters and wives) reported immense pressure, balancing care duties with household responsibilities, often with little family support.
Research Inclusion: women and low-income patients in Pakistan
We prioritised the voices of the most marginalised: women and low-income patients, who are rarely consulted in policy design. By documenting the “social death” feared by patients, we highlighted the need for culturally sensitive counselling that addresses social fears (e.g., marriage, isolation) alongside medical symptoms.
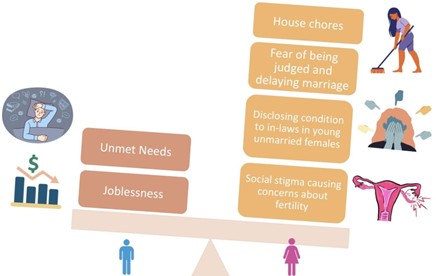
Gender dimension of TB-anxiety comorbidity
Project Impact
- The study provided the first qualitative evidence from Pakistan supporting the integration of anxiety care into routine TB services.
- We recommended formalising "counselling" into a structured intervention, including specific training for health workers to provide gender-sensitive psychological support.
Team
The project was led by Dr. Saima Afaq (University of York) in collaboration with:
- Valid Research Ltd (UK)
- Khyber Medical University (Pakistan)

The project’s operational and field team
Funder Information
This study was funded by the GCRF and Newton Consolidation Accounts (GNCAs) facilitated by the University of York, United Kingdom, (Ref No. MR/T037806/1).
