Articular Pilon Fracture Trial (ACTIVE)
What is a pilon fracture?
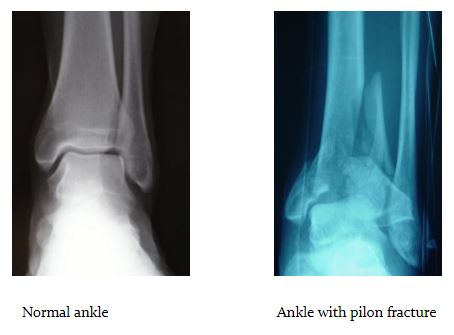
A pilon fracture is a particularly severe break of the shin bone where it forms the ankle joint (see X-rays). It is usually caused by high-energy impact such as a fall from a height. These injuries are very difficult to treat, because the force needed to break the bone in this way also causes considerable damage to the flesh, blood supply and nerves around it. Surgery is needed to fix the broken bone. Serious infections can occur after surgery, meaning more treatment is needed, including more surgery and on occasion amputation. Even where the fracture heals well, over time most patients develop arthritis in the joint. This injury can have a very large negative effect on a person’s quality of life.
Why is this study needed?
Pilon fractures are treated by orthopaedic surgeons. The injury is usually fixed from the inside (under the skin) using a plate and screws (called 'internal fixation'), or fixed from the outside using a ring frame or cage ('external fixation'). The internal plate is cheaper than the external ring but the internal plate may increase the chance of the patient getting a deep infection which could lead to more surgery. Both the National Institute for Health and Care Excellence (NICE) and Consultant Orthopaedic Surgeons in the UK have recommended that high-quality research is needed to find out whether internal or external fixation is best for treating pilon fractures and better use of NHS money.
What is the aim of the study?
The study aims to find out which of the two types of surgery is better in treating the injury, and in terms of costs. We will measure outcomes which have been chosen by National Institute of Clinical Excellence as critical or important for this question.
What type of study is this?
A randomised controlled trial comparing the outcomes of patients who receive internal plate fixation with those who receive an external fixation at 3, 6, 12 and 24 months from when the patient takes part in the study. We will assess the effects of the two types of surgery on patients' daily activities, quality of life, infection and unplanned further surgery. We will also investigate which procedure provides better value for money. We will do a qualitative study to explore issues around recruitment and monitor how well recruitment progresses in the first 12 months to make sure that the full trial is possible.
Who is being invited to take part?
We will include all adult patients (16 years or older in the United Kingdom, and 18 years or older in Australia and South Africa) with a type C pilon fracture of the tibia where the treating surgeon believes the patient will benefit from surgical fixation.
ACTIVE GDPR Transparency Information Sheet (PDF ![]() , 510kb)
, 510kb)
Privacy Notice: How we use your research data
Where is the study taking place?
NHS hospitals and specialist trauma centres in England, Scotland and Wales, and in public hospitals in Australia and South Africa. The three country-specific study protocols can be seen below.
United Kingdom - ACTIVE Trial Protocol (v4.0, 08.09.2021) (PDF ![]() , 1,480kb)
, 1,480kb)
Australia – ACTIVE Trial Protocol (v2.0, 24.09.2021) (PDF ![]() , 546kb)
, 546kb)
South Africa – ACTIVE Trial Protocol (v1.3, 14.02.2022) (PDF ![]() , 1,356kb)
, 1,356kb)
How to optimise recruitment into ACTIVE?
Consultations with our PPI panel, CRN leads and hospital sites have helped us to produce some simple advice sheets about how to identify and consent patients into ACTIVE. Please see the links below.
ACTIVE Guidance to sites about COVID-19 & Research from PPI (PDF ![]() , 635kb)
, 635kb)
ACTIVE Optimizing Identification of Patients (PDF ![]() , 721kb)
, 721kb)
ACTIVE Optimizing Patient Decision-Making (PDF ![]() , 939kb)
, 939kb)
Trial Details
Funder
National Institute for Health Research Health Technology Assessment Programme (15/130/84)
Sponsor
Hull University Teaching Hospitals
ISRCTN registration
ISRCTN98152560
IRAS project number
224065
Ethics Committee & Reference Number
Yorkshire & The Humber – Bradford Leeds REC 18/YH/0014
Start Date
01.09.2017
End date
30.04.2025
Contact Us
Please contact Dr Stephen Brealey(Trial Manager), stephen.brealey@york.ac.uk or call 01904 321357 if you have any enquires about the study.
YTU Team
Stephen Brealey - Trial Manager
Debbie Sykes - Trial Co-Ordinator
Jess Hugill-Jones - Trial Co-Ordinator
Lydia Flett – Trial Co-Ordinator
Ada Keding – Trial Statistician
Alex Mitchell – Statistician
Catriona McDaid – Co-applicant
Adwoa Parker – Co-applicant
David Torgerson - Co-applicant
Catherine Hewitt - Co-applicant
Joy Adamson - Co-applicant
External Collaborators
Mr Hemant Sharma - Chief Investigator, Hull and East Yorkshire Hospitals NHS Trust
Professor Matt Costa - Professor of Orthopaedic Trauma Surgery, University of Oxford
Mr Nikolaos Giotakis – Orthopaedic Consultant Surgeon, Royal Liverpool and Broadgreen University Hospitals Trust
Miss Elizabeth Barron - Clinical Lead Physiotherapist, Hull and East Yorkshire Hospitals NHS Trust
Mr Graham Gedney - Patient and public co-applicant